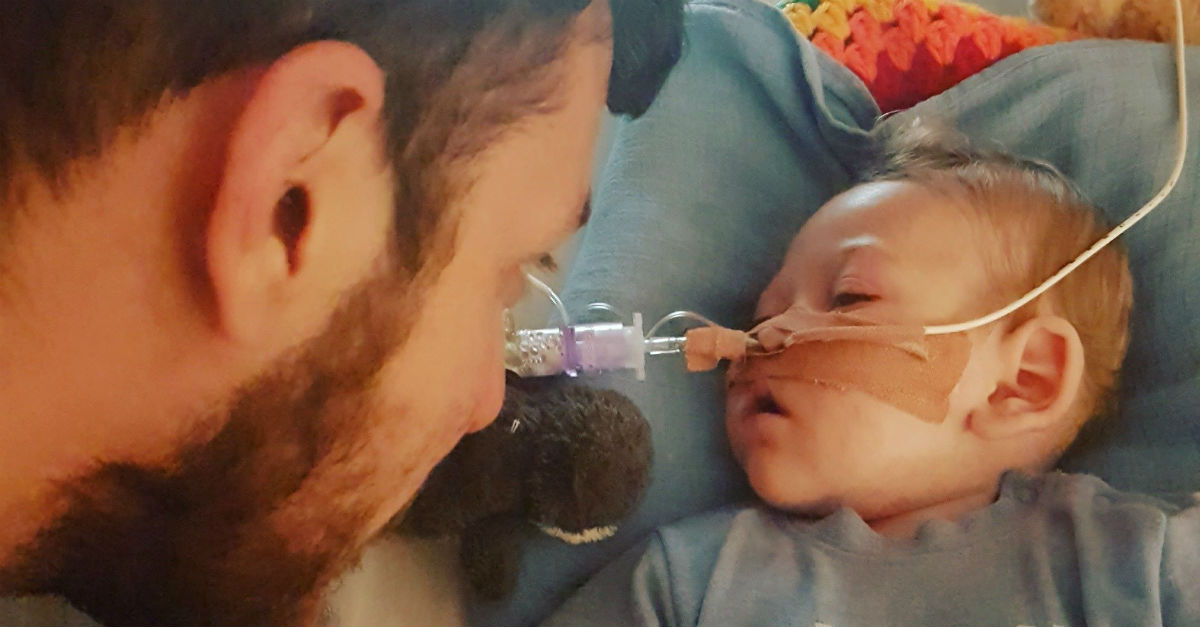
Charlie Gard is 11 months old and famous for all the wrong reasons. The British infant was born with infantile onset encephalomyopathy mitochondrial DNA depletion syndrome (MDDS), a rare genetic disease that is weakening his muscles and attacking his brain. At this stage, Charlie can’t breathe on his own—he requires a life support machine to stay alive—nor can he move his limbs or hold his eyes open. There is no known cure for his condition.
Videos by Rare
This situation would be grave under any circumstances, but it has drawn international attention because of the legal battle surrounding Charlie’s life. A hospital in the United States has an experimental treatment that could help the child, but because his parents sought treatment for him through a hospital that is part of the United Kingdom’s National Health Service (NHS), the British government has asserted its authority to deny them permission to try.
The family has lost several court appeals, but won the support of Pope Francis and President Trump. As of this writing, Charlie is still on life support. When you read this, that may no longer be true.
I confess that I’m late to the Charlie Gard story. By the time it caught my eye, most discussions were circling around one gutting question: Why?
Why is the NHS so set on limiting Charlie’s care?
Why can’t his family try an experimental treatment?
Why don’t his parents get to make their own decision?
RELATED: When government says your baby has to die
The answer to the first question is almost certainly to do with money. Nationalized health care systems ultimately have finite resources—resources they don’t want to use to prolong a terminal illness.
We see the same calculation in all state-run health systems. Here in the U.S., for example, Medicaid will not pay for nursing home care unless it is determined to be “medically necessary” for the patient. Likewise, Medicare has annual caps on what it will pay for certain physical therapies, which also must be “medically necessary.”
Setting aside all the hysteria over Obamacare “death panels,” this sort of limit is a reality when the government manages your medical system. It is how nationalized health care must work if it is to be even remotely fiscally responsible. Space prevents me delving deeper into the ethical and political implications of this fact, so suffice it to say Charlie Gard’s case is unusual in its drama and scale but, sadly, not a freak occurrence.
The answer to the second question involves what is in America known as the “right to try.” Some states have already passed “right to try” laws, which basically say that if a patient is suffering from a terminal illness, he can try treatments that aren’t proven effective or safe (the biggest issue here is allowing access to medicines the FDA hasn’t approved). Such laws are “all patient-driven,” explains Indiana State Representative Wes Culver, “because we have heard stories of people who are dying and there’s drugs out there that could possibly save them and they’re not allowed to take them and they’re like, ‘What have I got to lose?’”
In the Charlie Gard case, the NHS hospital has argued there “is significant harm if what the parents want for Charlie comes into effect.” This is exactly the illogic “right to try” opposes: When the alternative is death, the risk of “significant harm” may be your one shot at life. When credible doctors are offering the treatment and the patient’s family is supportive, it is Kafkaesque cruelty to deny the patient a chance.
RELATED: President Trump pledges to do what he can to aid a very sick baby
It is the third question, though, that is for me most pressing: Why don’t Charlie’s parents get to make their own decision about their son’s care?
NHS financial considerations here are irrelevant because Charlie’s parents independently raised about $1.7 million to cover the costs of prolonging his life. All the U.K. hospital must do is release the child to his mom’s and dad’s care. And though the NHS is probably correct that the experimental option won’t save Charlie’s life, that is not reason enough to stop his parents from trying. Again, all the NHS must do is get out of the way.
It’s true this is a complicated situation, and were I in Charlie’s parents’ shoes, I’d probably be more inclined to accept the limits of what medicine can accomplish. Their decision might not be mine. But I’m not in their shoes, and neither are the judges and bureaucrats who have quashed their requests—and that’s exactly why it shouldn’t be our call.